National Farm and Facility Level Biosecurity User Guide for the Equine Sector
Section 4: Principles of infection prevention and control programs
Infectious diseases in horses result from a complex interaction of three factors referred to as the disease triad:
- a horse that is susceptible to disease (the host);
- a pathogen such a bacterium, virus, fungus or parasite capable of causing disease (the agent);
- an opportunity for the host and agent to come into contact (the environment - which includes other horses and animals, the facility, food, water, soil, insects, equipment and humans).
Figure 5: The disease triad

Description for image – Figure 5: The disease triad
The diagram consists of a set of three overlapping circles of different colors. One circle contains the text host, one circle contains the text environment and one circle contains the text Agent. At the centre of the three intersecting circles is a yellow triangle with a yellow line on top representing a balance.
The disease triad illustrates that disease may result from the interaction of a susceptible horse (the host), a pathogen (the disease agent), and an environment favourable for disease development. There are many factors that influence whether disease will occur including the health of the animal, adequate nutrition, external stressors, the number of pathogens present and the ability of the pathogen to cause disease. However, there is a tipping point when sufficient factors overwhelm the ability of the animal to resist infection, tipping the balance in favor of the pathogen, which may allow disease to occur. Understanding the elements necessary for disease to occur provides the ability to influence and manage their impact to reduce disease. (Refer to Annex 2 and Annex 12 for information on equine diseases and parasites)
When discussing infection prevention, it is helpful to understand the distinction between infection and disease. Infection is the result of a pathogen invading and reproducing in a susceptible host. This does not always have an impact on the horse. Infection may lead to disease if there is a change from the normal function (for example damage to or a change in function of tissues and organs).
There are many host, agent and environmental variables that influence whether a horse will become diseased. Infection prevention and control programs rely on approaches that target these factors.
4.1 Sources of pathogens
- Horses that are infected but not showing signs of disease (a subclinical inapparent carrier or horse that has recovered from disease but still harbours the pathogen)
- Diseased horses
- Other domestic animals including pets
- Humans
- Food, water, and soil
- Equipment and other items (fomites)
- Housing areas and immediate surroundings
- Wildlife
- Pests (insects, spiders, ticks, rodents, birds and other animals that pose a nuisance to horses)


4.2 Methods of transmission
Pathogens can be transmitted (spread/transferred) by a number of routes; however, not all pathogens are transmitted by all routes. Pathogen characteristics, such as the ability to survive in the environment, can affect the mode of transmission.
- Direct transmission - Pathogens transmitted between animals through close physical contact.
- Direct contact - transmission through close physical contact between a susceptible animal and an infected animal, their bodily fluids or tissues. Depending on the pathogen, contact with skin, blood, saliva, respiratory fluids, urine, semen, fecal material and milk may result in transmission. In addition to the obvious modes of contact between individuals and groups, nose-to-nose contact over fences should always be considered.
- Indirect transmission - Some pathogens can be transmitted through an intermediate that has been contaminated and/or infected. This may be an inanimate object (a bridle, dirty clothing, contaminated feed and/or water) or a live animal (insect, rodent).
- Indirect contact - transmission through contact with people (for example, contaminated clothing, footwear, and/or hands), or with an inanimate object (fomite) through the shared use of equipment such as needles, syringes, artificial vaginas, dentistry equipment, contaminated vehicles, trailers, water buckets, and blankets. Pathogen transmission can occur over short distances (between animals on the same premises) and long distances (following travel to events and venues). Indirect contact with contaminated surfaces (dirty stalls and pens previously occupied by infected horses) can result in the transmission of pathogens. Pathogens transmitted by this route must be able to survive in the environment for the time required to come into contact with a susceptible horse.
- Ingestion - transmission by consuming feed and water contaminated by pathogens. The source of the contamination can include manure, urine, nasal discharge, and grass contaminated with parasite larvae.
- Aerosol transmission within a droplet - pathogens transmitted short distances by large fluid droplets generated by coughing, sneezing snorting and whinnying. Inhalation of these droplets can result in disease transmission.
- Airborne - transmission by very small particles that can be generated by disturbing contaminated materials. These can remain suspended in the air and travel over long distances.
- Vectors (living organisms) - transmission by a living organism (for example, people, animals, insects and ticks) infected with or contaminated by pathogens. In some instances, the insect vector is required for the development or multiplication of the pathogen prior to the pathogen being infective in the horse.
Figure 6: The status and spectrum of disease outcomes
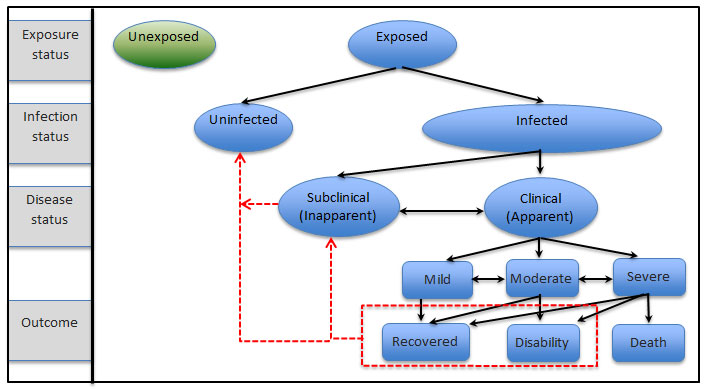
Description for image – Figure 6: The status and spectrum of disease outcomes
The diagram provides a visual depiction of the outcomes of exposunnnnnre to disease and or status of disease in horses. There are four rows to the diagram. In the top row from left to right is a box with the text "exposure status", an oval with the text "unexposed" and an oval with the text "exposed". Two arrows point from the oval with the word "exposed" to ovals in the row below it. On the far left of the second row is a box with the text "infection status". To the right of this is an oval with the text "uninfected" and to the right of this an oval with the text "infected" . From the box reading infected are two arrows pointing to the third row. On the far left of the third row is a box with the text "disease status". To the right of this are two ovals. The first oval contains the text "subclinical (inapparent) and the second oval contains the text "Clinical (apparent). There is a two headed arrow between the two ovals. From the oval "clinical apparent" are arrows pointing to 3 boxes below it that contain the text "mild", "moderate" and "severe". There are two headed arrows between the boxes "mild" and "moderate" and between "moderate" and "severe". The last row starting on the left contains a box with the text "Outcome". To the right of this are 3 rectangles. The first rectangle contains the text "recovered", the second rectangle contains the text "disability" and the third rectangle contains the text "death". The rectangle "recovered" has arrows coming to it from the rectangles "mild", "moderate", and "severe". The rectangle "disability" has arrows coming to it from "moderate" and "severe" and the rectangle "death" has an arrow coming to it from the rectangle "severe". The rectangles with the text "recovered" and disability have a dashed box around them with dashed arrows pointing back up to the oval with the text "subclinical inapparent" and the oval with the text "uninfected" There is also a dashed arrow from the oval with the text "subclinical inapparent" to the oval with the text "uninfected".
Figure 6: illustrates the status and outcome of an individual horse or a group of horses following disease exposure. When an individual horse or group of horses are exposed to a pathogen, many factors (for example, genetics, age, health status, and the type of pathogen) influence the outcome of the exposure. Healthy horses with a robust immune system may not become infected following exposure, others may become sub-clinically infected, and some horses may develop clinical sickness and never fully recover. Horses that have been clinically infected (visible signs of sickness) may go on to become subclinically infected (no visible signs of sickness yet they still carry the pathogen) or clear the infection and become uninfected.
In a group of horses, the diagram represents the various stages and outcomes of exposure to a pathogen that can be encountered at any one period of time. There can be a gradient with some horses remaining uninfected while other horses are at different stages; some are only recently exposed, others are clinically sick and some already recovered. After exposure, some animals may continue to harbour the pathogen even if they have recovered from disease (for example, Streptococcus equi [strangles] or equine herpes virus-1 [rhino]).
When normal biosecurity measures fail, horses may become infected with pathogens that require treatment. Treatment should always be conducted under the consultation and supervision of a veterinarian. The veterinarian is the person best able to prescribe the right drug for the condition at the right dose for the proper duration of time to effect a proper treatment and response.
4.3 General concepts of infection prevention and control
A) Decrease exposure to pathogens: This is the most important approach; eliminating contact between animals and pathogens prevents infection and disease. If exposure occurs, horses may become sick if there are enough organisms (an infectious dose) that can bypass the horses' defence systems and then multiply to cause disease. Many of the biosecurity practices focus on reducing exposure including: separating healthy horses from horses that are sick or of unknown health status, not sharing horse equipment and tack, eliminating contact between individuals or groups over fences and stalls, and cleaning and disinfecting housing areas for horses on a routine schedule and before use by a different horse.
i)
- Separation of new arrivals - Separate new horses and horses returning to a herd (for example, following a period off the property and exposed to other horses) until their health status is determined and/or specific preventive measures are applied (for example, deworming and vaccination).
- Separation of potentially higher risk horses - Identify horses that are a higher risk for harbouring and transmitting pathogens and manage them appropriately (separate and treat) to minimize the risk. This may include horses that are: visibly sick (clinical infection), known to have been exposed to sick horses, and those that have recently recovered from a sickness. Horses that are clinically sick require separation from other horses and must be managed with additional biosecurity measures.
- Separation of susceptible horses - Separate horses that are more susceptible (young, pregnant, senior) to infection from other horses.


ii) Cleaning and disinfection (for example, barns, stalls, alleyways, and trailers) - Perform routine cleaning and disinfection to reduce the number of pathogens that are present. Ideally, all pathogens should be destroyed and removed by cleaning and disinfection; however, this can be very difficult to achieve. Therefore, the goal is to reduce the pathogen level below that which is required to cause infection.
iii) Hand hygiene - Perform hand washing, use hand sanitizers, and when necessary use clean disposable gloves (washing hands or using hand sanitizer after removal of gloves) to minimize pathogen spread.


iv) Personal protective equipment - Change clothing and use protective outerwear (boots, coveralls and gloves) to provide a barrier to the transmission of pathogens. Personal protective equipment can be used to protect the health of your horse and your own health.
v) Access control - Manage access to the property and horses to limit exposure. Minimizing contact, particularly contact with non-resident horses and their owners or custodians, reduces opportunity for disease transmission to resident animals.

vi) Traffic flow - Manage opportunities for direct and indirect contact between horses, people, equipment, vehicles trailers and other materials on the property. Fences, gates, pathways and signage can assist in keeping things where they need to be.
vii) Pest management - Minimize pests by: decreasing attractants (cleaning up spilled food and preventing pooling of water in paddocks and fields), controlling access and locations for pests to establish populations (using window and door screens in barns and removing unnecessary equipment and debris), and actively controlling pests through traps, bait and insecticides or pesticides when necessary. Insecticides and pesticides should be used with caution and according the manufacturer's recommendations as some products can be harmful to horses if over dosed, other animals, humans and the environment.
viii) Pasture management - Manage pastures to minimize the accumulation and transmission of pathogens and parasites among horses. (For additional details refer to section 8.3)
B) Decrease susceptibility to disease: The best way to decrease susceptibility is to ensure your horse has a high health status. This can be accomplished in the following ways: Providing proper nutrition, managing underlying disease, reducing stress, implementing a good parasite a control program, controlling housing conditions (for example, temperature and humidity), providing proper dental care, managing pain, and ensuring the proper use of antibiotics and other medications. There are other factors that affect a horse's susceptibility to disease that cannot be influenced to a significant degree: age, sex, genetics, and pregnancy. Develop and implement a horse health management program.
C) Increase resistance to disease: Vaccination is the primary method used to improve resistance to certain infectious diseases. Vaccines need to be given and stored according to the label directions in order to be effective. Many vaccines require two or more doses to be effective; booster vaccinations to maintain protection are often required on a yearly or more frequent basis. Unfortunately, a small number of horses may not be protected by a vaccine because they fail to generate a sufficient immune response, or the vaccine has been compromised through improper handling or administration. Additionally, a small percentage of horses may not be able to be vaccinated for health reasons. To protect these animals, it is important that the majority of horses are vaccinated to stop the spread of disease. Develop a vaccination program and vaccinate horses against diseases using a risk based approach in consultation with your veterinarian.
Titer testing - It is now possible to determine the level of antibody to several diseases by testing a blood sample from a horse. This may help determine when revaccination is necessary for some diseases.
However, while antibody titers can provide some indication of the level of immunity (protection) to a disease, it only provides one part of the picture. The level of antibody (the titer) required to provide protection is still unknown for many diseases. Additionally, other components of the immune system that are important in defending against disease, such as cell mediated immunity, are not measured.
Titer testing may be appropriate in some situations for certain diseases, however there are limitations which should be discussed with your veterinarian.
D) Treatment with medications to control an infectious disease: There are many different medications that can be used to help manage infectious disease, thus decreasing the chances of it spreading to other horses. The medications most commonly used to control bacterial infections are antibiotics. Due to the risk of infectious organisms developing resistance to the various antibiotics and potential adverse effects (for example, diarrhea), antibiotics (and other medications) should be used with discretion and only under the direction of a veterinarian.
Poor biosecurity and inappropriate or indiscriminate drug use can lead to antimicrobial resistance, which has a significant effect on human and animal health
Records management - Good recordkeeping and written protocols provide the ability to instruct staff on appropriate protocols and improves consistency in horse management. Written records provide the ability to evaluate, verify and make adjustments to the biosecurity program over time. Important records include: vaccination, parasite control (deworming), health records, arrivals/departures, contact groups (for example pasture or paddock turnout groups, cleaning and disinfection protocols, protocols for dealing with sick or potentially infectious horses.
Additional resources on diseases and disease transmission:
- Date modified: